Au cours de chaque année académique, le département d’ophtalmologie organise, une série de 9 réunions scientifiques. L’objectif est de partager avec toute la communauté de l’ophtalmologie, des présentations de haut calibre, données par des spécialistes tant locaux qu’internationaux, invités à tour de rôle par les chefs de divisions.
Comité organisateur: Dr Patrick Hamel, professeur agrégé de clinique & Dre Isabelle Hardy, directrice du département de l’Université de Montréal.
Le département remercie l’Association des Médecins Ophtalmologistes du Québec pour son soutien financier.
Calendrier des prochaines réunions:
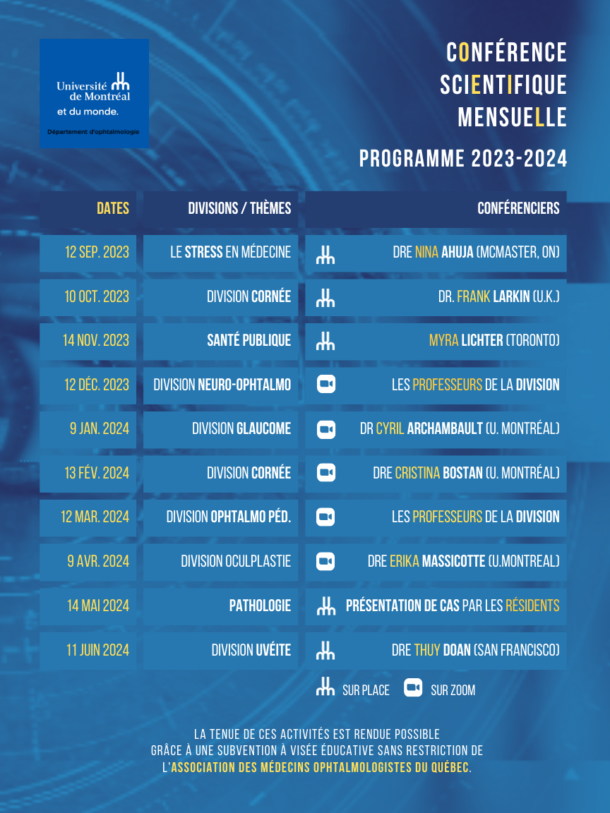
*** Le visionnement des conférences en différé ne donne pas le droit à des crédits ***
Saison 2023-2024
11 juin 2024
|
Uvéite |
 |
| “Beyond Traditional Tools: Unbiased Sequencing Approaches for the Diagnosis of Ocular Diseases”.
Présenté par la docteure Thuy Doan, MD, PhD (UCSF)
Dr. Thuy Doan, MD, PhD, is a uveitis specialist at the Proctor Foundation at the University of California, San Francisco (UCSF).
She obtained her MD at Stanford University and her PhD in Neurobiology & Behavior at the University of Washington, Seattle.
She directs a metagenomic epidemiology laboratory that utilizes innovative technical approaches and randomized controlled trials to understand how human microbiomes (ocular, gut, and upper respiratory tract) respond to clinically relevant perturbations.
In addition, her group uses genomic methods to efficiently identify infectious agents and biomarkers for ocular inflammatory diseases.
The laboratory is highly collaborative and works with international investigators from over 20 countries. Her work is funded by the National Eye Institute, the Bill & Melinda Gates Foundation, and the Research to Prevent Blindness.
|
 |
14 mai 2024
|
Histopathologie |
 |
| « Présentation de cas d’histopathologie par les résidents 5 »
Mikaël Bernier, Magaly Lacourse, Michael Trong Duc Nguyen et Milime Tondji Keyeutat (Université de Montréal) sous la direction du Dr. Miguel N. Burnier Jr, MD, MSc, PhD, FARVO (McGill).

Dr Miguel N. Burnier Jr, MD, MSc, PhD, FARVO
Director, Training & Development, RI-MUHC
The Thomas Hecht Family Chair in Ophthalmology (1995-2012),
Professor of Ophthalmology, Pathology, Oncology, Medicine, Surgery,
Director, The MUHC-McGill University Ocular Pathology & Translational Research Laboratory,
Director, The Melanoma Program, MUHC,
McGill University, Montreal, Canada.
|
 |
9 avril 2024
|
Oculoplastie |
 |
| « Approches transorbitaires à la neurochirurgie: qui, pourquoi, comment? ».
Présenté par la docteure Erika Massicotte de l’Université de Montréal.

Dre Erika Massicotte a complété son doctorat en médecine et sa résidence en ophtalmologie à l’Université de Montréal durant laquelle elle a été résidente-chef.
Elle a par la suite poursuivi une formation postdoctorale de 2 ans en oculoplastie à l’Université de Pittsburgh où elle a étroitement collaboré avec les services d’ORL et de neurochirurgie. Lors de son fellowship, elle a également travaillé en recherche fondamentale sur la reperfusion de l’artère ophtalmique chez les primates au sein de l’équipe du Dre Leah Byrne.
Dre Massicotte s’est jointe au service d’oculoplastie de l’Université de Montréal et au département d’ophtalmologie du Centre Hospitalier de l’Université de Montréal (CHUM) en 2021.
Elle a une passion pour l’enseignement et le travail multidisciplinaire. Dre Massicotte a un intérêt particulier pour la reconstruction des paupières, la chirurgie du système lacrymal et les cas complexes d’orbite.
|
 |
12 mars 2024
|
Ophtalmologie pédiatrique |
 |
| « L’implant Preserflo® MicroShunt chez l’enfant ».
Présenté par le docteur Patrick Hamel de l’Université de Montréal.

Après des études en médecine à l’Université Laval, puis en ophtalmologie à l’Université de Montréal, le Dr Patrick Hamel s’est surspécialisé en ophtalmologie pédiatrique à l’Université de Toronto, puis en glaucome à l’Université de Montréal.
Il œuvre en tant qu’ophtalmologiste pédiatrique au CHU Ste-Justine, à l’Hôpital de Montréal pour Enfants ainsi qu’au Centre Hospitalier de Rouyn-Noranda, avec un intérêt particulier en glaucome et en rétinoblastome.
Il est vice-doyen adjoint aux études médicales postdoctorales à l’Université de Montréal et président du comité d’examen en ophtalmologie du Collège royal des médecins et chirurgiens du Canada.
|
 |
13 février 2024
|
Cornée |
 |
| « La chirurgie de la cataracte après la chirurgie réfractive : une approche pratique ».
Présenté par la docteure Cristina Bostan de l’Université de Montréal.

Dr Cristina Bostan a complété le programme combiné de Doctorat en médecine et de Maîtrise en sciences biomédicales, suivi d’une Résidence en ophtalmologie à l’Université de Montréal, où elle a servi comme résidente-chef et a été nommée sur la Liste d’honneur de la Doyenne.
Elle a ensuite poursuivi un fellowship clinique et chirurgical en Cornée, maladies externes et chirurgie réfractive au Cole Eye Institute de la Cleveland Clinic.
Dr Bostan a également suivi une formation complémentaire de recherche en Cornée dans le cadre du Programme de formation de cliniciens-chercheurs et finalise actuellement une deuxième Maîtrise, notamment en Recherche Translationnelle à l’Université de Toronto.
Dr Bostan est maintenant cornéologue au Centre universitaire d’ophtalmologie de l’Université de Montréal à l’Hôpital Maisonneuve-Rosemont et Professeure Adjointe de Clinique à l’Université de Montréal.
|
 |
9 janvier 2024
|
Glaucome |
 |
| « Glaucoma in the UK: What I hope to bring to Montreal after training at Moorfields ».
Présenté par le docteur Cyril Archambault de l’Université de Montréal.

Le Dr Cyril Archambault est un ophtalmologiste pédiatrique et spécialiste en glaucome au CHU Sainte-Justine et à l’Hôpital Maisonneuve-Rosemont depuis 2023.
Il a complété sa résidence en ophtalmologie à l’Université de Montréal et a par la suite fait deux fellowships: le premier en ophtalmologie pédiatrique et strabisme à Stanford University (USA), et le deuxième en glaucome adulte et pédiatrique à Moorfields Eye Hospital à Londres (UK).
Il est le responsable de l’enseignement des externes, résidents et fellow en ophtalmologie au CHU Sainte-Justine depuis 2023. Ses intérêts cliniques principaux sont: le glaucome adulte et pédiatrique, la rétinopathie du prématuré et la cataracte pédiatrique.
|
 |
| 12 décembre 2023 |
Neuro-ophtalmologie |
 |
| « Pot-pourri de cas ».
Présenté par les docteures Katherine Boudreault, Caroline Gabias, Jacinthe Rouleau et Daniella Toffoli de la division de neuro-ophtalmologie de l’Université de Montréal.

Katherine Boudreault
Dr Boudreault a obtenu son doctorat en médecine à l’université de Montréal et sa licence du Conseil médical du Canada (LMCC). Puis elle s’est spécialisée en ophtalmologie à l’université de Montréal.
Elle a ensuite complété un fellowship en neuro-ophtalmologie au Massachusetts Eye and Ear, affilié à l’université Harvard à Boston. L’année suivante, elle a complété une deuxième surspécialité en électrorétinographie, génétique et dégénérescences rétiniennes à l’université Columbia à New-York.
Depuis, elle est professeure adjointe de clinique au département d’ophtalmologie de l’université de Montréal. Elle exerce la neuro-ophtalmologie et est responsable du laboratoire d’électrorétinographie du CHUM. Elle pratique aussi l’ophtalmologie générale et la chirurgie de la cataracte afin de conserver une pratique variée et stimulante. Elle est responsable de l’élaboration des grilles du stage de neuro-ophtalmologie pour les résidents du CHUM. Dr Boudreault s’implique activement dans la formation des externes, des résidents et des étudiants en optométrie.
Caroline Gabias
Dre Caroline Gabias est ophtalmologiste au CIUSSS NIM, principalement à l’Hôpital du Sacré-Cœur de Montréal. Elle est professeure adjointe de clinique à l’Université de Montréal.
Ayant d’abord obtenu un doctorat en optométrie à l’Université de Montréal en 2006, elle entreprend un doctorat en médecine et ensuite sa formation en ophtalmologie à l’Université de Montréal. Elle a par la suite complété sa formation par une année supplémentaire en neuro-ophtalmologie à University of British Columbia, à Vancouver.
Elle est impliquée dans la formation des externes et des résidents et aussi dans la formation des optométristes, de par sa participation aux cliniques d’ophtalmologie générale à l’Hôpital Maisonneuve-Rosemont et à l’Hôpital Notre-Dame.
Elle est aussi responsable du cours d’anatomie oculaire destiné aux étudiants de première année en optométrie de l’Université de Montréal.
Jacinthe Rouleau
La Dre Jacinthe Rouleau est ophtalmologiste et chirurgienne au CHUM. En plus d’avoir un poste de professeure adjointe de clinique à l’Université de Montréal.
Après avoir obtenu son doctorat en médecine à l’Université Laval, Dre Rouleau a complété sa formation en ophtalmologie à l’Université de Montréal. Elle a ensuite poursuivi sa formation par une année supplémentaire en neuro-ophtalmologie aux États-Unis, au réputé Department of Ophthalmology and Visual Science of Iowa.
En plus de la neuro-ophtalmologie, elle pratique l’ophtalmologie générale et porte un intérêt particulier pour la cataracte et le glaucome. Elle est une chirurgienne de la cataracte expérimentée et passionnée depuis 2007. Ses cliniques de neuro-ophtalmologie se font principalement au CHUM où elle est impliquée dans la formation des externes et des résidents. Contribuant également beaucoup à la formation continue, elle est régulièrement invitée comme conférencière dans différents congrès nationaux et internationaux, non seulement auprès de ses collègues ophtalmologistes mais aussi pour d’autres intervenants de la santé (optométristes, médecins de famille et médecins spécialistes).
Daniella Toffoli
Après avoir obtenu son diplôme en médecine de l’Université de McGill, Dre Daniela Toffoli a complété sa résidence en ophtalmologie à l’Université de Montréal. Elle a ensuite fait deux années de fellowship au Emory Eye Centre (Université Emory, Atlanta), premièrement en neuro-ophtalmologie puis en ophtalmologie pédiatrique.
Depuis 2012, Dre Toffoli travaille comme ophtalmologiste pédiatrique et neuro-ophtalmologiste à l’Hôpital de Montréal pour Enfants et au CHUM. Elle se spécialise également en strabisme adulte au CHUM. Elle est professeure adjointe à l’Université McGill et professeure associé à l’Université de Montréal. Depuis 2020, elle est directrice du programme de résidence à l’Université McGill. Elle s’implique activement dans l’enseignement des externes et résidents à l’Université McGill et à l’Université de Montréal. Elle est aussi la directrice médicale du Programme d’Intégration Francophone des Orthoptistes (PIFO) à l’Hôpital Montréal pour Enfants et participe en tant qu’examinatrice à l’examen National du Conseil Canadien d’Orthoptique.
|
 |
| 14 novembre 2023 |
Santé publique |
 |
| « GLOCAL Health Eye Care for the marginalized populations locally ».
Présenté par la docteure Myrna Lichter du Moorfields Eye Hospital et de l’UCL, Royaume-Uni.

Doctor Lichter : I graduated from the University of Manitoba with an MD and BSC (med) and was lucky enough to do my ophthalmology residency at University of Toronto. After residency I completed a fellowship at Armed Forces Institute of Pathology under the supervision of Dr. Lorenz Zimmerman and Dr. Ian Maclean.
Upon returning to Toronto, I started a comprehensive ophthalmology practice, and joined as an Outdoor Attending at Saint Michael’s Hospital. In 2000, when Saint Michael’s Hospital merged with the Wellesley Hospital, I was asked if I wanted to do an HIV screening clinic. It was there I started my clinic (soon morphing into a general clinic).It was at this clinic that I met a blind Native homeless patient, who profoundly influenced my direction. I felt it was amazing that this man, living on a bench in College Park would arrive at my Clinic on Tuesday afternoons. It was challenging experience, and I must admit I was not encouraged to continue the relationship. But it made me acutely sensitive to the difficulties faced by patients who were homeless.
In 2010, I received an Innovation Grant to try to deliver eye care to people homeless and marginally housed. My first student, Henry Fung, completed a needs assessment survey of primary care physicians. He also encouraged his friend Chris Noel, to continue the project, and that is when, with minimal supplies, we entered the shelters and stated to screen patients. Our first paper was published in JAMA and highlighted a pattern that we have seen repeatedly; that the incidence of visual problems was about 25%; 6X the national average.
We went on to study homeless youth, families living in shelters (with Dr. Nasrin Tehrani). I received a very generous grant, and purchased more sophisticated equipment, so we were now prepared to offer glasses to homeless patients (paid by my grant) and I was able to hire an assistant. We have subsequently reached out to homeless women, people living “rough” (Out of the Cold”), and even examined patients during COVID, setting up tents in Moss Park. We explored cataract surgery, and issues surrounding treating HMH patients. In all we have published about 16 papers. In 2015, I was approached by a student, Tarek Bin Yameen, who was moved by the plight of Syrian refugees.
With the help of Islamic Institute of Toronto, PRISM Eye Institute and KEI, we were able to hold five clinics, examining approximately 800 newcomers. They were given eye examinations, and glasses. Have just finished our Afghanistani refugee screening clinics, seeing about 350 Afghan refugees.
Just before COVID, we decided to look at the Indigenous homeless population, and have seen about 100 homeless Indigenous people. With respect to CAPO rules, we will soon be publishing our results. The other very exciting project in collaboration with Sick Children’s Hospital and Native Child and Family Services, will be our vision screening for Native children. The mission is that every child should be tested and get glasses if needed.
My next avenue ( I hope) will be the establishment of a sustainable centre for vision testing for homeless patients, and long term follow up. I also have an interest in remote vision testing, and the use of smartphone technologies.
My other eye related interests include sitting on EDI committee, executive of Canadian Association for Public Health and Global Ophthalmology at COS, and of course teaching and learning from the students that have been integral to every part of this journey. I feel that we learn as much from the courage of the patients we see as we give back to them. It has been an honour to meet many of them. I hope that the students I have worked with will not abandon this mission as they move forward.
I do have a few other interests, including baking (we did doing a fundraiser, cookie decorating at Walter Wright – hopefully an annual event); Yoga – my passion for many years; and of course my new cat who has joined us on many ZOOM meetings.
|
 |
| 10 octobre 2023 |
Cornée |
 |
| « Management of Karatoconus in young patients».
Présenté par le docteur Frank Larkin du Moorfields Eye Hospital et de l’UCL, Royaume-Uni.

Professor of Corneal Diseases, University College London and consultant at Moorfields Eye Hospital, where he holds three referral clinics weekly in adult and paediatric cornea and external diseases.
His research has mainly concerned corneal transplantation, ranging from experimental models to graft outcomes in patients.
Since 2012 he has chaired the OTAG Audit & Clinical Research sub-group which advises NHS Blood & Transplant and has published over 30 national transplant outcome audits in international journals.
He has more recently been leading early phase and randomised trials in corneal disorders and was director of the NIHR Moorfields Clinical Research Facility 2012-21.This is the world’s largest eye and vision research CRF and has supported several first-in-man studies.
He has been editor-in-chief of the British Journal of Ophthalmology since 2021.
|
 |
| 12 septembre 2023 |
Stress en médecine |
 |
| « Managing stress in Medicine ».
Présenté par la Dre Nina Ahuja de l’Université McMaster d’Hamilton, ON.

After graduating from McMaster University Medical School, Dr. Nina Ahuja completed her residency in ophthalmology at University of Ottawa in 2003. She started her surgical practice in Hamilton and was a key contributor in establishing the ophthalmology residency program at McMaster resurrected in 2005. Throughout her career, Dr. Ahuja has held several leadership roles in hospitals and academic institutions, including President of the Medical Staff Association at St. Joseph’s Healthcare Hamilton, Residency Program Director followed by Academic Division Head for ophthalmology at McMaster University, and President of the Association of Canadian University Professors of Ophthalmology (ACUPO). She has been an active member of several executive committees including the Board of Governors at St. Joseph’s Healthcare Hamilton. Dr. Ahuja is currently on the Board of Directors for St. Joseph Healthcare Foundation, member of the Canadian Ophthalmological Society’s EDI Working Group, and an examiner for ophthalmology for the Royal College of Physicians and Surgeons of Canada.Drawing from her experiences as a frontline healthcare provider, private practice owner, educator and physician leader in both academic and healthcare organizations, in 2019 Dr. Ahuja founded Docs in Leadership to deliver emotionally intelligent leadership curriculum that supports EDI principles, and aligns with CanMEDS non-medical expert roles. She is a certified emotional intelligence coach and has received numerous awards for teaching excellence and contributions to medical education. She was recently presented with the 2023 Women in Ophthalmology Champion for Change Award from the Canadian Ophthalmological Society recognizing her work in EDI, positive physician culture and leadership development.
Dr. Ahuja is a happily married “bonus mom” and also author of bestselling book, “Stress in Medicine: Lessons Learned Through My Years as a Surgeon, from Med School to Residency, and Beyond”. She enjoys spending time with her family, and continues to write on the unique joys and stresses of high achievers for Psychology Today in her blog, “Striving High”.
Dr. Ahuja is committed to advancing physician education in emotional intelligent leadership and well-being, through her comprehensive Docs in Leadership programs and podcast appearances in Canada and the US.
|
 |
Saison 2022-2023
| 13 juin 2023 |
Oculoplastie |
 |
| « A Day in the Life of a Pediatric Orbit Surgeon ».
Présenté par le docteur Vikram Durairaj de la Dell Medical School, Austin, TX.
Dr. Vikram David Durairaj was raised in Central Texas where both his physician parents practiced medicine for over 25 years. He graduated from Trinity University with a degree in Biology and a minor in Biophysics. While attending medical school at the University of Texas Health Science Center, he was elected to Alpha Omega Alpha, the national medical honor society. Dr. Durairaj completed his Internship at Georgetown University and his Residency at the University of Colorado. He completed his 2-year American Society of Ophthalmic Plastic and Reconstructive Surgery Fellowship at the Mayo Clinic in Rochester, Minnesota.
Dr. Durairaj has performed over 20,000 eyelid, orbit and lacrimal surgeries. He currently serves as Managing Partner of TOC Eye and Face and is Professor of Ophthalmology at the Dell Medical School – University of Texas at Austin. Dr. Durairaj is the Director of the American Society of Ophthalmic Plastic and Reconstructive Surgery Fellowship and Preceptor of the AACS Facial Cosmetic Surgery Fellowship at TOC Eye and Face.
Dr. Durairaj has given over 400 invited national and international lectures and courses, published over 200 peer-reviewed manuscripts, chapters, and abstracts, and presented his research at national and international meetings. He has served as editor and reviewer for 18 scholarly publications. He has been selected to US News and World Report Top Doctors, America’s Top Ophthalmologists, Best Doctors in America, Texas Super Doctors, TX TopDocs and Best Doctors in Austin. In 2011, he received the achievement award from the American Academy of Ophthalmology and served as Program Chair for the American Society of Ophthalmic Plastic and Reconstructive Surgery.
|
 |
| 9 mai 2023 |
Neuro-ophtalmologie |
 |
| « Cas mystères d’œdème des nerfs optiques ».
Présentés par les docteurs Katie Luneau, Francine Mathieu Millaire, Kinda Najem, Luis Ospina et Jacinthe Rouleau de l’Université de Montréal.

Dre Katie Luneau
Docteure Luneau a obtenu son doctorat en médecine à l’Université Laval, puis son diplôme de spécialité en ophtalmologie à l’Université de Montréal. Elle a complété par la suite une surspécialisation (fellowship) en neuro-ophtalmologie à l’Université Emory à Atlanta aux États-Unis (Emory University School of Medicine). Docteure Luneau est professeure d’enseignement clinique à la Faculté de médecine de l’Université de Montréal. Elle travaille depuis 2008 au Centre Hospitalier de l’Université de Montréal (CHUM).
Dre Francine Mathieu Millaire
Courte biographie (avril 2023)
Ophtalmologiste, spécialisée en neuro-ophtalmologie
Hôpital Maisonneuve-Rosemont (1978- )
CHUM (1999- ) (Hôpital de la Cité-de-la-Santé (2021- )
Hôpital Sacré-Cœur (1980-2021) Hôpital Ste-Justine (1985-2010), Hôpital de Gatineau (2010-2019).
Études médicales et résidence à l’Université de Montréal.
Fellowship neuro-ophtalmologie au Wilmer Institute, John Hopkins Hospital, Baltimore.
Prix et Honneurs :
1969 : Bourse: meilleur étudiant section Biochimie, Collège Jean-de-Brébeuf
1976 Bourse Percy Hermant pour meilleur résident en ophtalmologie.
1978-1979 Récipiendaire de la Bourse de la Fondation MacLaughlin, pour sa formation en neuro-ophtalmologie à l’Hôpital John’s Hopkins, États-Unis.
2016 : Nommée « Membre Émérite » de la FMSQ (Fédérations des Médecins Spécialistes du Québec) pour sa grande contribution à l’histoire de la FMSQ
2017 : Honorée par l’AMOQ (Association de Médecins Ophtalmologistes du Québec) pour l’ensemble de son œuvre.
Université de Montréal
Membre élu Conseil Faculté de Médecine 1999-2002
Membre du comité prix, bourses et autres distinctions 2002-2009.
Collège Royal Médecins Chirurgiens du Canada
Membre du jury d’examen en ophtalmologie 1988-1992
Présidente du jury d’examen ophtalmologie 1992-1995
Association Ophtalmologistes du Québec (AMOQ)
Présidente élue: 1994-1996 et 2003-2005
Fédérations Médecins Spécialistes Québec (FMSQ)
Vice- présidente élue FMSQ 2001-2003
Présidente Comité régional Montréal 1995-2002
Membre élue Conseil d’administration 1997 -2003
Comité de révision des médecins spécialistes 1998-
Association Canadienne Protection Médicale (ACPM)
Administrateur élu 2005-2014
Comité sur l’étendue de l’assistance
Comité de révision des dossiers
Collège Médecins Québec (CMQ)
Administrateur élu 2014 – 2022
Présidente groupe travail médecine esthétique
Présidente groupe travail en phlébologie
Comite activités médicales partageables
Comité révision des plaintes
Présidente comité Ordre Dentistes du Québec – Collège des Médecins
Commission de la santé et de la sécurité au travail (CNESST)
2002 – Médecin-expert du Bureau d’évaluation médicale (BEM)
PAAB Pharmaceutical Advertising Advisory Board)
Membre nommé du conseil d’administration (2002-2003)
Autres
1995-2002 Membres Conseil de rédaction Journal Médecine Sport
1995-1998 Membre, Comité conjoint sur l’exposition aux rayons UV
En plus de nombreuse présentations, conférences, articles, chapitres de livres et participations à de nombreuses émissions de télévision et radio.
Dre Kinda Najem
Docteure Kinda Najem est neuro-ophtalmologiste au CUO-Hôpital Maisonneuve-Rosemont et y travaille depuis 2016. Elle a fait ses études de médecine et sa résidence en ophtalmologie à l’Université de Montréal et a complété un fellowship en neuro-ophtalmologie à l’Université de Toronto. Elle a également effectué une maîtrise en pédagogie médicale au MGH Institute of Health Professionals et au Harvard Macy Institute à Boston. Docteure Najem est professeur d’enseignement clinique à la Faculté de Médecine de l’Université de Montréal.
|
 |
| 18 avril 2023 |
Histopathologie |
 |
| « Présentation de cas d’histopathologie par les résidents 5 ».
Présenté par nos résidents de 5e année: Fares Antaki, Jessica El Khazen Dupuis, Simon Javidi, Oksana Kaminska et Guillaume Mullie (Université de Montréal) sous la direction du Dr. Miguel N. Burnier Jr, MD, MSc, PhD, FARVO (McGill).

Dr Miguel N. Burnier Jr, MD, MSc, PhD, FARVO
Director, Training & Development, RI-MUHC
The Thomas Hecht Family Chair in Ophthalmology (1995-2012),
Professor of Ophthalmology, Pathology, Oncology, Medicine, Surgery,
Director, The MUHC-McGill University Ocular Pathology & Translational Research Laboratory,
Director, The Melanoma Program, MUHC,
McGill University, Montreal, Canada.
|
 |
| 14 mars 2023 |
Pédiatrie |
 |
| « Cas intéressants en pédiatrie »
Présentés les docteurs Patrick Hamel, MD, FRCSC, Ashwaq Bin Amro, MD, Charlotte Lussier, MD (Université de Montréal) et Marwa Al Ghafri (Université McGill)

Patrick Hamel : Ophtalmologiste pédiatrique, professeur agrégé et vice-doyen adjoint aux études médicales postdoctorales à l’Université de Montréal ainsi que professeur adjoint à l’Université McGill, ainsi que chef du service d’ophtalmologie au CHU Ste-Justine. Études médicales à l’Université Laval, suivies d’une résidence en ophtalmologie à l’Université de Montréal, d’un fellowship en ophtalmologie pédiatrique à l’Université de Toronto et d’un second fellowship en glaucome à l’Université de Montréal. Le Dr Hamel œuvre particulièrement au CHU Ste-Justine, ainsi qu’à l’Hôpital de Montréal pour Enfants et au CISSS de l’Abitibi-Témiscamingue, en ophtalmologie pédiatrique avec une intérêt particulier en glaucome pédiatrique et en rétinoblastome.
Ashwaq Bin Amro : Pediatric ophthalmology and strabismus fellow at UdeM.
Charlotte Lussier : Résidente de 3e année en ophtalmologie à l’Université de Montréal où elle a aussi complété son doctorat en médecine.
Marwa Al Ghafri : Marwa Al Ghafri is an ophthalmology resident (PGY3) at McGill University.
|
 |
| 7 février 2023 |
Compétence par conception |
 |
| « Déjouer les pièges liés à la mise en place de la CPC, optimiser l’utilisation des APC au quotidien et mettre en place un comité de compétences fonctionnel »
Présenté le docteur Tareck Ayad, MD, FRCSC, (Université de Montréal)

Dr Tareck Ayad est ORL et chirurgien cervico-facial au CHUM et à HMR avec une pratique centrée sur l’oncologie et la reconstruction. Il est professeur titulaire à l’Université de Montréal et directeur de programme d’ORL. Sa recherche est axée sur l’oncologie, la chirurgie de reconstruction et l’évaluation objective du geste chirurgical. Il est président du comité de recherche du YO-IFOS (Young Otolaryngologists – International federation of Otorhinolaryngology Societies).
|
 |
| 10 janvier 2023 |
Chirurgie |
 |
| « Quand les lentilles intraoculaires nous jouent des mauvais tours. »
Présenté le docteur Georges Durr, MD, FRCSC, (Université de Montréal)

Le Dr Durr a complété sa formation en médecine et sa résidence en ophtalmologie à l’Université de Montréal. Il a poursuivi sa formation de deux ans en glaucome et chirurgie de segment antérieur complexe à l’Université de Toronto avec le Dr Ike Ahmed. Il pratique présentement au Centre Hospitalier de l’Université de Montréal (CHUM) où il traite une panoplie de pathologies en passant du glaucome, à la cataracte et aux chirurgies de complexe du segment antérieur.
Ses activités de recherche s’étendent aux nouvelles chirurgies en glaucome et en cataracte. D’ailleurs, il chapeaute plusieurs projets sur des nouvelles thérapies en glaucome et en chirurgie de cataracte. Il a publié dans de nombreuses revues et il a deux chapitres de livre à son actif. Dr Durr enseigne également aux étudiants en médecine et aux résidents et il est directeur du programme de fellowship en glaucome à l’Université de Montréal.
|
 |
| 13 décembre 2022 |
Rétine |
 |
| « Clin d’œil sur la réalité virtuelle en rétine et en ophtalmologie. »
Présenté le docteur Karim Hammamji, (Université de Montréal)

Docteur Hammamji est spécialiste et chirurgien vitréo-rétinien (rétine médicale et chirurgicale).
Il est aussi professeur adjoint à la clinique du Centre Hospitalier de l’Université de Montréal (CHUM) et fait partie de l’équipe d’oncologie oculaire en tant que responsable des chirurgies complexes associées au cancer de l’œil.
Ses champs d’expertises incluent la dégénérescence maculaire, la rétinopathie diabétique, et les maladies d’interfaces vitréo-rétinienne (trou maculaire, membrane épirétinienne, et traction vitréo-maculaire)
Le Dr Hammamji a fait sa formation médicale à l’Université McGill, et sa résidence en ophtalmologie à l’Université de Montréal. Il a ensuite poursuivi une formation de 2 ans en chirurgies et pathologies de la rétine, à l’Université de Calgary, et au centre d’ophtalmologie prestigieux du Moorfields Eye Hospital à Londres.
Au cours de sa carrière, il s’est dévoué à la recherche et au développement de sa spécialité. Il est présentement chercheur au Centre de Recherche du CHUM (CRCHUM). Il a fait de multiples présentations scientifiques locales et internationales, et a été lauréat de plusieurs prix et bourses pour son travail.
Il est également Chef de la division Rétine de l’Université de Montréal et directeur du programme de fellowship en chirurgie vitréo-rétinienne.
|
 |
| 8 novembre 2022 |
Cornée |
 |
| « Real world outcomes of endothelial keratoplasty ».
Présenté la docteure Divya Srikumaran, (Wilmer Eye Institute, MD, USA)

Divya Srikumaran, M.D, is an associate professor of ophthalmology in the Division of Cornea and External Disease at the Johns Hopkins Wilmer Eye Institute. She received her M.D. degree from Northwestern University Feinberg School of Medicine, after which she completed her ophthalmology residency and cornea fellowship training at the Wilmer Eye Institute. Dr. Srikumaran’s research interest includes the assessment of corneal transplant outcomes and risk factors for receiving keratoplasty through big data sources including administrative claims data. She received the Hoskins Center IRIS Registry Research Fund Award through the American Academy of Ophthalmology as well as the EBAA Pilot Research grant to study real-world endothelial keratoplasty outcomes. She is busy clinician who is actively involved in several multi-center clinical trials. In addition, she is member of the board of the Cornea Society and serves on the scientific program committee of the EBAA and is participating in their Physician Leadership Program. She is also a member of the editorial board for Cornea and Eye and serves an associate editor for the Cornea Society’s new journal Cornea Open. She is also a renowned educator and currently serves as Vice Chair of Education and was previously residency program director. As vice chair of education, she has an interest in medical education and studying best practices to support doctors in training. Blending her passion for both education and expertise in corneal surgery, Dr. Srikumaran has also studies barriers to adoption of advanced keratoplasty procedures in the US and abroad. Dr. Srikumaran also an examiner and member of the cornea and cataract exam content development committees for the American Board of Ophthalmology and mostly she was selected to participate in their Visiting Scholar Program.
|
 |
| 18 octobre 2022 |
Uvéite |
 |
| « Ocular lymphoma – a wolf in sheep’s clothing ».
Présenté la docteure Fatma Zaguia, (Département d’ophtalmologie, Université de Montréal)

Dr Zaguia completed her medical degree and a Master’s degree in Neuro-Immunology at McGill University in Montreal. She then went on to complete her Ophthalmology residency at McGill University in 2020. She completed a fellowship in Uveitis and Ocular Immunology at Northwestern University in Chicago, Illinois. She is currently an assistant professor at McGill University, as well as an associate member at the Centre Hospitalier de l’Université de Montréal. Her expertise includes the medical and surgical care of uveitis in adult patients. She is also actively involved in teaching medical students and residents at both centers, and currently holds the position of Chair of the Competence Committee for the residency program at McGill University.
|
 |
| 13 septembre 2022 |
Glaucome |
 |
| « Aqueous Dynamics & Glaucoma ».
Présenté le docteur Sheng Lim, (King’s College London, Royaume-Uni)

Sheng Lim is the head of the glaucoma service at St Thomas’ Hospital and Professor of Glaucoma Studies at King’s College London. He is also the research lead for the ophthalmology department and the head of KCL Frost Eye Research Department at St Thomas’ Hospital.
He qualified from University of Leicester Medical School and trained in general ophthalmology and glaucoma in London during the residency and fellowship program. He obtained his research MD degree from University College London based on his research in glaucoma surgery devices. He had been the International Glaucoma Association Post-doctoral fellow at the Mayo Clinic, Rochester, Minnesota, under the supervision of Drs Brubaker and Johnson.
His current research interests are exclusively in human aqueous dynamics and treatment for glaucoma.
|
 |
Saison 2021-2022
| 14 juin 2022 |
Troubles immunitaires et infectieux de l’oeil |
 |
| « Astuces dans la gestion des viroses oculaires ».
Présenté le docteur Marc Labetoulle, (Hôpitaux universitaires Paris-Sud)

Marc Labetoulle,
M.D., Ph.D., FEBO
Professeur d’Ophtalmologie, Université Paris-Saclay
Chef du Service d’Ophtalmologie, CHU Bicêtre, Le Kremlin-Bicêtre, France
Après avoir obtenu son diplôme de Médecin spécialiste en Ophtalmologie en 1994 à l’Université Paris-Descartes au décours immédiat de son résidanat en tant qu’Interne des Hôpitaux de Paris (1989-1993), il a occupé successivement les postes de Chef de Clinique (1995-1999), d’Assistant de Recherche (1999-2000), de Maître de Conférence en Thérapeutiques (2001-2006) puis de Professeur en Ophtalmologie (2006-). Parallèlement à ses études en Médecine, il a aussi suivi un cursus complet en sciences biologiques, option microbiologie, et a été Lauréat du cours de Virologie Fondamentale de l’Institut Pasteur (Paris, 1994). Il a ensuite passé 2 ans comme chercheur à temps plein (1994-1995 et 1999-2000) au sein du Département de Virologie du CNRS (Gif-sur-Yvette), où il était Responsable de l’équipe « Latence HSV ».
Titulaire de la chaire d’Ophtalmologie de l’Université Paris-Sud depuis 2009 ; son équipe de recherche a rejoint le Centre d’immunologie des infections virales et des maladies auto-immunes (IMVA, CEA,Université Paris Sud, Inserm U1184), où il poursuit désormais ses recherches expérimentales sur l’équilibre entre latence et réactivation du virus Herpes simplex de type 1 (HSV1) dans le système nerveux puis dans les tissus oculaires, tout en continuant d’avoir une activité clinique, tant médicale que chirurgicale, de façon quotidienne, au CHU de Bicêtre (Paris-Saclay), dans l’équipe de soins qu’il encadre.
Son implication constante dans un mode d’exercice transversal (du lit du patient au laboratoire et inversement) lui a permis de jouer un rôle passionant dans le domaine des troubles immunitaires et infectieux de l’œil, en particulier ceux de la surface oculaire (cornée et conjonctive). Il est par exemple impliqué depuis 20 ans dans le suivi des patients Sjögren inclus dans la cohorte de l’Hôpital Bicêtre (Centre National de la maladie de Sjögren, coordonné par le Pr Xavier Mariette), et son équipe a aussi été labélisée Centre National de référence pour les herpès oculaires sévères. Il a participé à plus de 50 essais cliniques (internationaux, randomisés, contrôlés), dont 8 en tant qu’Investigateur Principal. Il est l’auteur de plus de 220 publications internationales revues par des pairs et référencées dans PubMed. Son équipe vient récemment d’être invitée à donner le cours sur les kératites herpétiques aux Sub-Speciality Days de l’American Academy of Ophthalmology.
|
 |
| 10 mai 2022 |
Résidence |
 |
| « Compétence par conception ».
Présenté le docteur Christian Loubert, (Université de Montréal)

Ayant terminé un doctorat en médecine à l’université de Montréal ainsi qu’une résidence en anesthésiologie à la même université, Dr Loubert a complété sa formation par un fellowship en recherche clinique en anesthésiologie obstétricale à Londres, au Royaume-Uni. Son expertise et son intérêt pour l’anesthésie obstétricale l’ont amené à publier plusieurs articles scientifiques et à être conférencier invité dans plusieurs congrès nationaux et internationaux.
Dr Loubert est aussi impliqué dans l’enseignement aux résidents, notamment en siégeant depuis 2013 au comité de programme en anesthésiologie de l’université de Montréal à titre de responsable des résidents de l’hôpital Maisonneuve-Rosemont et comme président du comité de compétence depuis 2016. Il continue à développer une expertise concrète en la matière puisque que le programme d’anesthésiologie compte maintenant 5 cohortes de résidents qui poursuivent leur formation médicale par compétence. Il siège de plus sur le comité facultaire des étude médicales post-doctorales pour l’implantation de la compétence par conception, sur le comité de suivi des compétence aux études médicales pré-doctorales de l’université de Montréal et est membre du comité exécutif de la communauté des présidents de comités de compétence de l’université de Montréal.
|
 |
| 5 avril 2022 |
Histopathologie |
 |
| « Présentation de cas d’histopathologie par les résidents 5 ».
Présenté par nos résidents de 5e année: Maude Anderson, Olivier Fontaine, Joseph-Raymond Hakim, Taylor Nayman, Andrei-Alexandre Szigiato. (Université de Montréal)

Anderson, Maude
maude.anderson@umontreal.ca
MD – Université de Sherbrooke (2017)
Fontaine, Olivier
olivier.fontaine@umontreal.ca
Hakim, Joseph Raymond
joseph-raymond.hakim@umontreal.ca
Nayman, Taylor
taylor.nayman@umontreal.ca
MD, CM – Université McGill (2017)
Szigiato, Andrei-Alexandru
andrei-alexandru.szigiato@umontreal.ca
B.Sc. – York University (2012)
MD – University of Toronto (2016)
Glaucoma and Advanced Anterior Segment Surgery (GAASS) Research Fellowship – U. of Toronto, Prism Eye Institute (2017)
|
 |
| 8 mars 2022 |
Intelligence artificielle |
 |
| « Artificial Intelligence in Ophthalmology: Going from Code to Clinic ».
Présenté par le Dr Pearse Keane (University College London, UK)
Pearse Keane is Professor of Artificial Medical Intelligence at UCL Institute of Ophthalmology, and a consultant ophthalmologist at Moorfields Eye Hospital, London. He is originally from Ireland and received his medical degree from University College Dublin (UCD), graduating in 2002.
In 2016, he initiated a formal collaboration between Moorfields Eye Hospital and Google DeepMind, with the aim of developing artificial intelligence (AI) algorithms for the earlier detection and treatment of retinal disease. In August 2018, the first results of this collaboration were published in the journal, Nature Medicine. In May 2020, he jointly led work, again published in Nature Medicine, to develop an early warning system for age-related macular degeneration (AMD), by far the commonest cause of blindness in many countries.
In October 2019, he was included on the Evening Standard Progress1000 list of most influential Londoners (https://www.standard.co.uk/news/the1000) and in June 2020, he was profiled in The Economist (https://www.economist.com/technology-quarterly/2020/06/11/the-potential-and-the-pitfalls-of-medical-ai).
In 2020, he was listed on the “The Power List” by The Ophthalmologist magazine, a ranking of the Top 100 most influential people in the world of ophthalmology (https://theophthalmologist.com/power-list/2020).
|
 |
| 8 février 2022 |
Rétine |
 |
| « Le rétinoblastome en temps de COVID en France ».
Présenté par la Dr Nathalie Cassoux (Institut Curie, Paris FR)
Nathalie Cassoux is medical Director at Institut Curie in Paris and head of ocular oncology department. She obtained a MD, a master 1 on molecular oncology and immunology and a master 2 and PhD degrees on bio informatics at Pierre et Marie Curie Paris 6 university. She is full professor in Ophthalmology, chair ocular oncology at the University de Paris. She was elected at the board of Curie foundation. She is in the board of the French Society of Ophtalmology (SFO) and past president of the European Oncology Group (OOG). She’s author or coauthor of 183 peer-reviewed articles. She received an Award of the American Academy of Ophthalmology on 2010 and Award of French society of Ophthalmology on 2011.
Clinical activities are focused on ocular tumors (retinoblastoma, uveal melanoma, conjunctival and eyelids tumors and ocular lymphoma). The research interests are focused on translational ocular oncology (genetic of ocular tumors, animal models, preclinical assessment). She coordinates at Institut Curie a research team on orthotopic xenografted models of ocular tumors and participates to multidisciplinary group of scientists and doctors devoted to uveal melanoma and retinoblastoma research. She is part of molecular oncology lab UMR 144 CNRS
|
 |
| 14 décembre 2021 |
Cornée |
 |
| « Refractive Surgery: The Art, Science, and Philosophy ».
Présenté par le Dr Kashif Baig (Université d’Ottawa)
Dr. Kashif Baig, a Cornea, Anterior Segment, Cataract, and Refractive Surgeon, is the Founder/Medical Director of Precision Cornea Centre, Medical Director at Herzig Eye Institute Ottawa, and Assistant Professor at the University of Ottawa Eye Institute.
He completed his medical and residency training at McGill University, MBA Degree at McMaster University, and Fellowship training in the United States.
Dr. Baig has a strong interest in the development, and implementation of surgical innovations in corneal and anterior segment surgery.
|
 |
| 9 novembre 2021 |
Oculoplastie |
 |
| Démystifier la fenestration des gaines du nerf optique.
Présenté par Dre Erika Massicotte (Université de Montréal)
Dre Erika Massicotte a complété son doctorat en médecine et sa résidence en ophtalmologie à l’Université de Montréal durant laquelle elle a été résidente-chef.
Elle a par la suite poursuivi une formation postdoctorale de 2 ans en oculoplastie à l’Université de Pittsburgh où elle a étroitement collaboré avec les services d’ORL et de neurochirurgie.
Lors de son fellowship, elle a également travaillé en recherche fondamentale sur la reperfusion de l’artère ophtalmique chez les primates au sein de l’équipe du Dre Leah Byrne.
Dre Massicotte s’est récemment jointe au service d’oculoplastie de l’Université de Montréal et au département d’ophtalmologie du Centre Hospitalier de l’Université de Montréal (CHUM).
Elle a une passion pour l’enseignement et le travail interdisciplinaire. Dre Massicotte a un intérêt particulier pour la reconstruction des paupières, du système lacrymal et de l’orbite.
|
 |
| 12 octobre 2021 |
Équité, Diversité, Inclusion |
 |
| Conférence spéciale: Équité, Diversité, Inclusion
Présenté par Dre Margaret Henri (Université de Montréal)
Chirurgie générale au CIUSSS de l’est de l’ile (HMR)
MD 1996 UdeM
Chirurgie 2001 UdeM
Directrice de programme MD UdeM depuis oct 2019
Répondante pour la faculté de médecine en matière de EDI -RPP (secrétariat général UdeM) nov 2020
|
 |
| 14 septembre 2021 |
Glaucome |
 |
| Chères zonules, qu’avez-vous fait de mon angle?
Présenté par Dr Paul Harasymowycz (Université de Montréal)
Fondateur et Directeur Médical des cliniques d’Ophtalmologie Bellevue et de l’Institut de Glaucome de Montréal et Professeur Associé à l’Université de Montréal, le Dr. Harasymowycz travaille comme clinicien et chercheur au Centre Universitaire d’Ophtalmologie au Centre de recherche Guy-Bernier depuis 2001. Il a été Chef de Glaucome à l’université de Montréal pour plus de 12 ans et est membre de Faculté du International Congress of Glaucoma Surgery. Il est également Directeur médical de la Fondation du Glaucome du Québec créée en 2007 qui pour but de promouvoir la recherche sur cette maladie et sensibiliser la population afin d’encourager les personnes à risque d’effectuer un dépistage précoce.
Dr.Harasymowycz est membre du comité de glaucome au ASCRS (American Society of Cataract and Refractive Surgery) et le GERSO, et ACUITI et juge international au XOVA Excellence in Ophthalmology Vision Award. Il concentre ses recherches sur les nouvelles techniques diagnostiques en glaucome, incluant l’imagerie de l’oeil et traitements chirurgicaux en glaucome, en chirurgie de la cataracte et segment antérieur.
De plus, il est souvent appelé à présenter et enseigner les nouvelles techniques et traitements chirurgicaux à des congrès nationaux et internationaux, et est un des pionniers des chirurgies micro-invasives en glaucome (MIGS).
Depuis plus de 20 ans, le Dr.Harasymowycz se démarque par ses multitudes recherches et au delà de 70 publications dans diverses revues scientifiques au niveau national et international, ainsi que pour ses chapitres de livre sur le glaucome. Expert et passionné, il enseigne à des externes, des résidents, des fellows, et autres professionnels de la santé .
|
 |
Saison 2020-2021
| 11 mai 2021 |
Rétine |
ROP in low and middle income countries: Challenges and Opportunities.
Présenté par Professor Clare Gilbert (London School of Hygiene & Tropical Medicine, UK)
Professor Clare Gilbert MB ChB., FRCOphth., MD., MSc, trained in surgical retina and worked as a clinical ophthalmologist in the UK for 10 years. She has worked at the International Centre for Eye Health at the London School of Hygiene & Tropical Medicine, UK since 1990. Her main research interest is blindness in children in low and middle income countries, including refractive errors, ROP, cataract and primary eye care. She has undertaken studies in collaboration with colleagues in Latin America, Africa and Asia.Clare is a technical advisor to several non-government organizations including the Vision Impact Institute, the USAID Child Blindness Program, and until recently, the Queen Elizabeth Diamond Jubilee Trust (the Trust). She has provided technical advice to two large scale programmes in India for ROP and diabetic retinopathy supported by The Trust.Clare has facilitated over 30 workshops on ROP across Latin America and in Vietnam, Central Europe, Ukraine, Russia, Pakistan and Bangladesh. She was a member of a group who contributed to PAHO’s Guidelines on ROP for South and Central America, and is chairing ICOs working group who will develop global ROP guidelines.Clare is an author of almost 350 peer reviewed publications (more than 50 on ROP), and has written 26 book chapters. She has received several international awards, including the Jules Francois Golden Award (ICO), and International Prevention of Blindness Award (AAO) and the Barrie Jones Award (Royal College of Ophthalmology).
|
 |
| 9 mars 2021 |
Histopathologie |
Présentation des résidents R5 « Corrélations histopathologiques de cas cliniques ».
Présenté par nos résidents de 5e année: Cyril Archambault, Cristina Bostan, Sarah Chorfi, Marie-Pier Matton et Louis Vaillancourt. |
 |
| 9 février 2021 |
Uvéite |
Infectious retinitis: not everything in uveitis is treated with steroids.
Présenté par Dre Debra A. Goldstein (Northwestern University Feinberg School of Medicine, Chicago)
Debra Anne Goldstein, MD, FRCSC
Magerstadt Professor of Ophthalmology
Director, Uveitis Service
Director, Uveitis Fellowship
Department of Ophthalmology
Northwestern University Feinberg School of MedicineDr. Debra Anne Goldstein received her medical degree from McGill University in Montreal, Canada, where she subsequently completed an ophthalmology residency. She then pursued a fellowship in uveitis and ocular immunology at McGill followed by a second fellowship in uveitis at the University of Illinois at Chicago. Dr. Goldstein has published over 250 peer-reviewed papers and book chapters and has lectured widely all over the world. She has conducted extensive investigator initiated and multicenter research projects. She has been the recipient of numerous awards and honors including the Senior Achievement Award from the American Academy of Ophthalmology, the Life Achievement Honor award from the American Academy of Ophthalmology, the AAO Secretariat Award for special contributions to the Academy, Unsung Hero recognition from the AAO, as well as an AOA clinical teaching award. She was twice awarded the Golden Apple Award for Best Teacher in Ophthalmology when she was a professor at the University of Illinois at Chicago. In April of 2017 she was awarded the prestigious Magerstadt Professorship in Ophthalmology. In 2021 she became an ARVO Silver Fellow. Dr. Goldstein is currently the Magerstadt Professor of Ophthalmology as well as the Director of the Uveitis Service in the Department of Ophthalmology at Northwestern University’s Feinberg School of Medicine.
|
 |
| 12 janvier 2021 |
Uvéite |
Update on masquerade syndrome and vitreoretinal lymphoma.
Présenté par Dre Elisabetta Miserocchi (San Raffaele Scientific Institute, Milan, Italy)
Elisabetta MiserocchiSan Raffaele Scientific Institute, Milan, ItalyProfessor Elisabetta Miserocchi is a Consultant Ophthalmologist of the Ocular Immunology and Uveitis Service, based at University Hospital San Raffaele Milan, Italy in the department of Professor Francesco Bandello. After graduating with a medical degree from the University of Milan in 1996, Professor Miserocchi completed a four-year residency in the Department of Ophthalmology at the San Raffaele Scientific Institute, including a 2 two year research fellowship at the Massachusetts Eye and Ear Infirmary, part of Harvard Medical School, Massachusetts, USA with Dr. Stephen Foster.Her main areas of interest and activity are diagnosis and treatment of uveitis, pediatric uveitis associated with rheumatic diseases, ocular cicatricial pemphigoid, herpetic ocular disease. And intraocular lymphoma. Professor Miserocchi is also currently participating to many international multicentre clinical trials on systemic immunosuppressive agents for non infectious uveitis. Professor Miserocchi is a member of the International Uveitis Study Group and the American Uveitis Society. Professor Miserocchi is widely published in peer-reviewed journals and has presented her work at a number of national and international congresses; she was awarded the SOI-SOE Lecture at the Società Oftalmologica Italiana 2012 annual meeting in Rome for new treatments in non-infectious uveitis, and she received the American Academy of Ophthalmology Award in 2015. Dr Miserocchi has conducted research and applied new therapies to further the diagnosis and treatment of non-infectious uveitis.
|
 |
| 2 décembre 2020 |
Rétine |
Thérapie génique de la mutation héréditaire du gène RPE65 : Une première au Canada!
Présenté par Dre Cynthia Qian et Dr Flavio Rezende (UMontréal)
Dre Cynthia Qian, MD, FRCSCEmail: cynthia.xin-ya.qian@umontreal.ca
Publications: PubMed
Clinical Interests: Surgical retina, Adult and pediatric retinal diseases; Inherited retinal diseasesCynthia X. Qian est professeure adjointe au département d’ophtalmologie et chef du laboratoire d’électrophysiologie et de la section rétine pédiatrique de l’Université de Montréal. Dr. Qian a terminé ses études en médecine à l’Université McGill. Elle a ensuite poursuivi sa résidence à l’Université de Montréal où elle a été élue résidente en chef. Elle a gradué en tant que valédictorienne sur la liste de la Doyenne. Elle est doublement formée en fellowship de rétine chirurgicale au Massachusetts Eye and Ear Infirmary du Harvard Medical School et en maladies héréditaires de la rétine au Kellogg Eye Center de l’Universitee de Michigan.
Elle est actuellement vice-présidente de la Société Canadienne de la rétine et la représentante provinciale pour le Québec en ophtalmologie sur le comité de surspécialité du Collège royal des médecins et chirurgiens du Canada.Ses principaux intérêts de recherche portent sur les essais cliniques sur de nouvelles thérapies dans les maladies héréditaires de la rétine. Elle est experte sur les pathologies de la rétine pédiatrique et les dystrophies rétiniennes, en particulier sur l’implantation chirurgicale des prothèses rétiniennes et l’administration sous-rétinienne de thérapie génique.
Dr. Qian est reconnue pour son travail novateur en tant qu’étoile montante en ophtalmologie clinique, chirurgicale, et en recherche. Elle a été élue « Jeune professionnelle de l’année » par la Jeune Chambre de commerce de Montréal en 2018 et comme lauréate du Top 40 under 40 au Canada en 2019.
Dr Flavio Rezende, MD, PhD
Dr Flavio Rezende, Md. PhD est professeur agrégé de clinique au Département d’ophtalmologie de l’Université de Montréal, et Ophtalmologiste chirurgien vitreo-retinien au Centre universitaire d’ophtalmologie de l’Hôpital Maisonneuve-Rosemont
En tant que professeur agrégé du Département d’ophtalmologie de l’Université de Montréal (UdeM), je dirige le volet clinique / chirurgical de notre équipe de recherche translationnelle au Centre Universitaire d’Ophtalmologie, Hôpital Maisonneuve-Rosemont (CUO-HMR), Montréal, Québec , Canada. Mon objectif principal est la prise en charge chirurgicale des maladies vitréo-rétiniennes compliquées, l’enseignement universitaire et la recherche translationnelle chirurgicale.
En tant que chirurgien vitréo-rétinien, j’ai développé et amélioré des techniques chirurgicales complexes pour gérer les maladies vitréo-rétiniennes. J’ai également développé des techniques chirurgicales pour obtenir des biopsies vitreuses en milieu ambulatoire, fournissant du matériel instrumental pour notre unité de recherche en biologie neuro-vasculaire. Nous construisons actuellement une bio-banque d’échantillons d’humeur vitreuse et aqueuse.
En tant que chercheur translationnel en chirurgie, depuis 5 ans, je suis impliqué dans l’implant Retinal Chip, développant une technique chirurgicale innovante pour une puce rétinienne de nouvelle génération.
Sur le plan académique, j’ai été chargé du programme de bourses vitréo-rétiniennes du Service de la rétine, Département d’ophtalmologie, UdeM pendant 5 ans (2013-2018).
Et au cours de la dernière année, j’ai occupé le poste de directeur clinique au CUO-HMR et, à ce titre, je me suis engagé à apporter davantage d’innovation au profit de nos patients. Des projets en cours feront de notre centre universitaire d’ophtalmologie, l’un des premiers centres au Canada de thérapie génique pour des affections rétiniennes auparavant incurables.
|
 |
| 10 novembre 2020 |
Glaucome |
MIGS: L’embarras du choix!
Présenté par Dre Susan Wakil, Dre Qianqian Wang et Dr Georges Durr (Université de Montréal)
Dre Susan Wakil, MD, FRCSC
Dr Wakil a complété ses études médicales et sa résidence en ophtalmologie à l’Université de McGill sur la liste d’honneur du Doyen. Elle a par la suite complété sa formation de surspécialité en glaucome chirurgical au centre renommé de l’Université Duke en Caroline du Nord, E-U, ou elle a obtenu le prix « Hornaday Fellow of the Year Award ». Lors de sa deuxième année à l’Université Duke elle a travaillé en tant que clinicienne associée et a entamé un fellowship de recherche portant sur plusieurs sujets tels l’intelligence artificielle, les chirurgies du glaucome et la génétique du glaucome en Afrique. Elle complète actuellement une maîtrise en Santé Publique avec l’Université de Hopkins, E-U. Elle est professeur adjoint de clinique à l’Université de Montréal et pratique principalement à l’Hôpital Sacré-Cœur de Montréal ainsi que dans d’autres centres hospitaliers.
Dre Qianqian Wang, MD, FRCSC
Après avoir obtenu son doctorat en médecine à l’Université McGill, Dre Qianqian Wang a poursuivi sa formation en ophtalmologie à l’Université de Montréal. Elle a ensuite complété sa formation de surspécialité en glaucome chirurgical au renommé Hôpital Wills Eye à Philadelphie, É.-U. À son retour à Montréal, elle a également complété un fellowship en recherche sur la neurorégénération au laboratoire de la Dre Adriana Di Polo au Centre de Recherche de CHUM. Dre Wang est l’auteure de nombreux articles scientifiques et présente régulièrement aux congrès nationaux et internationaux. Elle est professeur adjoint de clinique à l’Université de Montréal et pratique au CHUM, Clinique Ophtalmologique Berri et Hôpital Lachine. Son champ d’intérêt inclut les traitements médicaux et chirurgicaux traditionnels et innovants en glaucome ainsi que la recherche clinique en glaucome.
Dr Georges Durr, MD, FRCSC
Dr Durr a complété son baccalauréat, sa médecine et sa résidence en ophtalmologie à l’Université de Montréal. Il a obtenu son bac en sciences biomédicales sur la liste d’honneur du Doyen. Par la suite, il a poursuivi sa formation avec un fellowship de 2 ans en Glaucome et Chirurgie Complexe du Segment Antérieur à l’Université de Toronto en autre sous la tutelle du Dr Ike Ahmed. Ses activités de recherche touche surtout les nouvelles innovations en glaucome, cataracte et la reconstruction du segment antérieur. Présentement, il pratique à l’Université de Montréal au CHUM (Centre Hospitalier Universitaire de Montreal). Il est professeur adjoint de clinique et directeur du fellowship en glaucome à l’Université de Montréal.
|
 |
| 20 octobre 2020 |
Oculoplastie |
Bench to Bedside: Evolution of Therapy for Thyroid Associated Ophthalmopathy
Présenté par Dr Terry Smith (Kellogg Eye Center)
Terry J. Smith, M.D.
Frederick G.L. Huetwell Professor of Ophthalmology and Visual Sciences
Professor, Department of Internal Medicine
Kellog Eye Center
University of Michigan
Biography
Dr. Terry J. Smith, the Frederick G.L. Huetwell Professor in Ophthalmology and Visual Sciences at the University of Michigan, is an internationally-known endocrinologist who has studied Graves’ disease, its eye manifestations, and related autoimmune disease for over 20 years. Dr. Smith’s laboratory was first to describe the unique molecular attributes of tissue surrounding the eye that make it susceptible to inflammation in Graves’ disease. He has identified a novel autoantibody that binds to and activates a specific receptor, resulting in an exaggerated autoimmune response. His investigation of these mechanisms has yielded several potential therapeutic targets that may interrupt the disease process. These will provide the focus for future clinical trials.
Dr. Smith received his medical degree from the University of Missouri School of Medicine and completed his residency at the University of Illinois in Chicago and Sinai Hospital in Baltimore. He has completed fellowships in biophysics at the University of California School of Medicine, San Francisco, in molecular biochemistry at Columbia University in New York, and clinical endocrinology at the Pritzker School of Medicine, University of Chicago.
Dr. Smith is the author of over 150 articles and book chapters, and has been awarded five patents for his research discoveries. He has been elected to the Orbit Society, is chief scientific officer for the National Graves’ Foundation, and serves as reviewer for numerous scientific journals. Dr. Smith has been funded continuously by the National Institutes of Health and the Veterans Administration since 1983.
Areas of Interest
Research Areas
Clinical Trials – Eye Plastics
Research Summary
Autoimmune thyroid disease, extracellular matrix, cell signaling, gene expression, ecosanoids, inflammation and cytokine action
Dr. Smith’s laboratory group is interested in understanding and developing new treatments for Graves’ Disease (GD) or thyroid-associated ophthalmopathy (TAO).
Graves’ Disease is an autoimmune process directed primarily at the thyroid. Many of the patients with GD also exhibit inflammation of the tissues around the eye. Orbital manifestations of GD known as TAO, involve the dramatic remodeling of connective tissues surrounding the eye. Alterations in orbital tissue architecture can adversely affect the function and health of the eye in several ways.
- They can deprive the globe of normal irrigation and eyelid coverage, leading to chronic irritation and infection.
- They can compromise the ability of the eyes to move in a coordinated fashion, restricting motility, and resulting in disconjugate gaze and diplopia.
- They can cause cosmetic changes that sometimes exert a profoundly deleterious impact on the psychological health of afflicted patients.
- They can threaten eye sight by compressing the neuro-vascular supply to the eye.
There are no specific safe and effective therapies for TAO. Our overall goal is to identify the molecular and cellular mechanisms responsible for the pathogenesis of orbital involvement in TAO. We have found that patients with TAO have dramatically increased numbers of circulating fibrocytes. These fibrocytes derive from stem cells originating in the bone marrow. They infiltrate the connective tissues of the orbit. We believe that the phenotypic attributes of orbital fibroblasts underlie the propensity of the tissues surrounding the eye to become involved in GD. As a direct consequence of identifying the peculiarities exhibited by these cells, we are now in a strong position to create strategies for interrupting the disease process at a very early stage.
Their work is focused on defining the molecular targets that will lead to effective and specific therapy design.
Clinical Interests
Graves’ disease, thyroid-associated ophthalmopathy, metabolic diseases
Specialties: Endocrinology, Internal Medicine
Honors & Awards
2018
- Merit Award, University of Missouri School of Medicine
- Clinical Trial, A Phase 3, Randomized, Double-Masked, Placebo-Controlled, Parallel-Group, Multicenter Study Evaluating Teprotumumab (HZN-001) Treatment in Subjects with Active Thyroid Eye Disease (OPTIC) – INC Research/Horizon Pharma USA, Inc.
2017
- River Vision Pilot Study; River Vision
Credentials
- Medical School – University of Missouri School of Medicine, 1975
- Residencies
- Department of Medicine, University of Illinois, Chicago, IL, 1976
- Department of Medicine, Sinai Hospital, Baltimore, MD, 1977
- Fellowships
- Biophysics, Cardiovascular Research Institute, University of California School of Medicine, San Francisco, CA, 1978
- Biochemistry, Columbia University, New York, NY, 1979
- Endocrinology, Pritzker School of Medicine, University of Chicago, Chicago, IL, 1981
Published Articles or Reviews
View a list of publications on Michigan Experts
Source = https://medicine.umich.edu/dept/ophthalmology/terry-j-smith-md
|
 |
| 15 septembre 2020 |
Cornée et segment antérieur |
Cataract Surgery in Patients with Corneal Disease: Pearls and Pitfalls.
Présenté par Dr Anthony J. Aldave (UCLA)
Anthony J. Aldave, M.D.
Professor of Ophthalmology
Walton Li Chair in Cornea and Uveitis
Chief, Cornea and Uveitis Division
Director, Cornea and Refractive Surgery Fellowship
The Stein Eye Institute
Anthony J. Aldave, MD, received his medical degree from the University of Texas Medical Branch in Galveston. He performed his residency training in ophthalmology at the Wills Eye Hospital, Thomas Jefferson University, in Philadelphia, Pennsylvania. Dr. Aldave then completed a two-year Cornea, Uveitis and Refractive Surgery Fellowship at The University of California, San Francisco/ Francis I. Proctor Foundation. He joined the Stein Eye Institute in July 2002 as a full-time member of the Cornea and Refractive Surgery Services. Dr. Aldave is currently a Professor of Ophthalmology, holds the Walton Li Chair in Cornea and Uveitis, is Chief of the Cornea and Uveitis Division and Director of the Cornea and Refractive Surgery Fellowship Program.
Dr. Aldave has received numerous honors during his career, including the Alpha Omega Alpha Scholarship Award for graduating first in his medical school class, the Heed Ophthalmic Foundation Fellowship, the American Ophthalmological Society-Knapp Testimonial Fund Fellowship, the first Claes Dohlman Society Award, and the Achievement, Secretariat and Senior Achievement Awards from the American Academy of Ophthalmology.
In addition to his busy clinical practice, Dr. Aldave directs the Corneal Genetics Laboratory at the Stein Eye Institute. Dr. Aldave’s laboratory research focuses on the molecular genetics of the corneal dystrophies, a group of inherited disorders that affect corneal clarity and constitute one of the primary indications for corneal transplantation. Recognized as a leader in his chosen field of scientific investigation, Dr. Aldave has authored over 150 peer-reviewed scientific publications, has been invited to give almost 450 scientific presentations at local, national and international meetings and serves as a scientific reviewer for 19 ophthalmology and genetics journals.
|
 |
Saison 2019-2020
| 9 juin 2020 |
Cornée et segment antérieur |
La chirurgie de la cataracte bilatérale simultanée.
 Présenté par Dre Marie-Ève Légaré (Université Laval) Présenté par Dre Marie-Ève Légaré (Université Laval)
|
 |
















































![]()







 Présenté par Dre Marie-Ève Légaré (Université Laval)
Présenté par Dre Marie-Ève Légaré (Université Laval)

















